Steroid Injections – Benefits, Risks and Alternatives
Steroid injections are an anti-inflammatory treatment for a wide range of painful joint and soft tissue conditions. They are often used to alleviate pain in inflammatory and degenerative joint and soft tissue conditions, such as rheumatoid arthritis, osteoarthritis, bursitis, and tendinitis. This article explores what steroid injections are, how they work, and what you can expect during and after a steroid injection treatment. Furthermore, we touch on alternative treatment and injection options.

What Are Steroid Soft Tissue Injections?
Steroid injections involve delivering a concentrated dose of the anti-inflammatory medicine directly to the site of inflammation. A small needle, the size of a blood test needle, is used to administer the steroids. This can achieve a strong therapeutic effect on a specific area or joint, thereby avoiding side effects associated with the regular use of steroid tablets. Steroid injections can be highly effective where pain is localised to one or two specific areas or joints rather than widespread. To increase the efficacy of the treatment, it is often performed as an ultrasound-guided injection where a radiologist uses real-time ultrasound imaging to confirm the correct needle placement before the injection is administered.
Conditions Treated with Steroid Injections
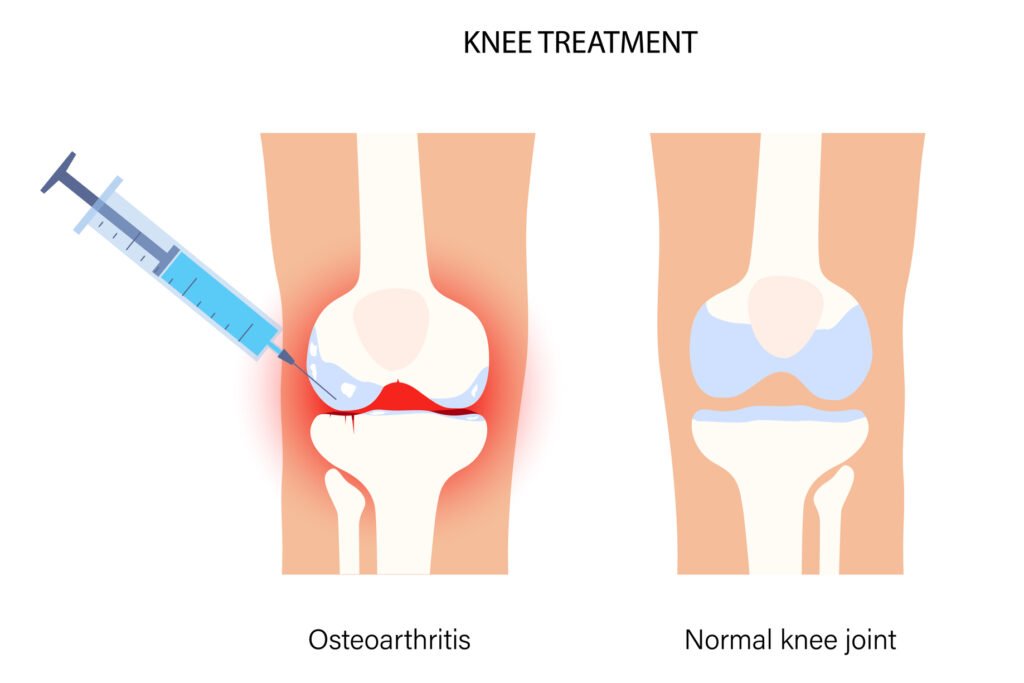
Steroid injections are used to treat a wide range of conditions, including:
- Arthritis: Inflammatory arthritis (e.g., rheumatoid arthritis) and osteoarthritis.
- Bursitis, for example, subacromial bursitis of the shoulder and greater trochanteric bursitis at the outer aspect of the hip.
- Tendinitis or tendinosis, for example, supraspinatus tendinosis of the shoulder. It can be used around other tendons around the wrist, elbow and the ankle, but the indication for this should be carefully considered by your doctor.
- Frozen shoulder, often in conjunction with a hydrodistension of the shoulder
- Plantar fasciitis.
- Trigger finger. Steroid injections can be used alone, or in conjunction with ultrasound-guided trigger finger release.
- Carpal tunnel syndrome.
These injections are particularly effective for conditions where inflammation is a key component of pain and dysfunction.
How Steroid Injections Work
Steroids used for injections are a synthetic form of corticosteroids, which are naturally present in the human body. Steroids can reduce inflammation by inhibiting the production of inflammatory chemicals, reducing the activity of immune cells and reducing capillary permeability [1]. The two most used types of steroids are methylprednisolone and triamcinolone. These are long-acting preparations. The onset of action for intra-articular methylprednisone occurs at 1 week and lasts 1 to 5 weeks[1]. The maximum effect of steroids occurs between the first and second weeks and it gradually fades off over a few months. In conditions where steroids are used to treat inflammation without much structural damage, for example, bursitis in the shoulder, or tendonitis, a steroid injection can potentially have a longer-lasting effect, especially when combined with physiotherapy. In osteoarthritis, where structural damage to the joint prevails, steroids cannot heal or reverse the damage but still play an important role in pain management.
The Injection Procedure
The procedure for administering steroid injections is relatively straightforward:
- The radiologist will perform an ultrasound scan to confirm the diagnosis.
- The injection site is cleaned with an antiseptic solution.
- In most cases, a local anaesthetic is injected to numb the area. This part of the procedure may sting a little, but the needle is of the same size as a needle used for routine blood tests
- The steroid medication is then injected. For precise placement of the injection, imaging guidance may be used, where the precise needle position can be confirmed.
The procedure usually takes only a few minutes.
Benefits of Steroid Soft Tissue Injections
The primary benefits of steroid injections include:
- Rapid pain relief, often within 24 to 48 hours
- Reduced inflammation in the targeted area
- Improved joint mobility and function
- Localised treatment with fewer systemic side effects compared to oral steroids (i.e. tablets).
These benefits can significantly improve a patient’s quality of life and ability to perform daily activities.
Potential Side Effects and Risks of Steroid Injections
While steroid injections, if performed only occasionally, are generally considered a safe treatment, there are potential risks and side effects[2]. Some of the risks are related to the steroid medication itself, and some are related to the injection procedure.
Side effects of steroid injections include:
- Postinjection flare is an exacerbation of pain after injection. Approximately one-third of patients experience some initial worsening of the pain, which usually only lasts a couple of days [3]
- Infection is very rare (less than 0.001%).
- Tendon, ligament, or fascial insufficiency or rupture (very rare for single injections).
- Skin hypopigmentation and atrophy (more so if injected under the skin rather than into a joint).
- Facial flushing
- Headaches and insomnia
In some cases, the steroid injection may fail to alleviate the symptoms or may do so only for a very short time.
Although joint injections are a focal treatment, some amount is absorbed by the bloodstream. Due to its nature as a hormonal medicine, steroids have a wide range of effects, including on blood pressure, blood sugar level, the adrenal glands, body weight and mood. Most of these effects are only relevant in patients with pre-existing medical conditions or if steroids are given in high doses. It is therefore best to discuss this with your doctor.
More recently, concern has been raised regarding the risk of progression of arthritis with cartilage loss and bone injury after steroid injections. However, one of the studies reporting acceleration of arthritis, patients received serial knee joint injections every 12 weeks over two years[4], which is more than common practice in most places. There remains uncertainty over the long-term benefits of steroid joint injections[5], [6], a recent review concluded that
“Intraarticular GC injections are not associated with an increased risk of knee OA progression compared to hyaluronic acid.”[7]
How long do steroid injections last
The effectiveness of steroid injections can vary depending on the condition being treated and individual factors. Many patients experience significant pain relief lasting anywhere from a few weeks to several months. However, it’s important to note that steroid injections are not a cure-all solution and may not be effective for everyone. Factors affecting treatment success include:
- The specific condition being treated
- The severity of inflammation
- The patient’s overall health
- Proper injection technique
How long the effect of a steroid injection lasts depends on the body part and on which condition is being treated.
- For knee joint, pain relief after a steroid injection to the knee joint lasts on average around 3 months[7]. The effect peaks 2 weeks after the injection and then gradually wears off.
- For the treatment of subacromial impingement syndrome in the painful shoulder, steroid injections last between 3 and 6 months[8].
There is variation in how the patient responds to an injection. The same injection in different patients can lead to a different experience.
Alternatives to Steroid Injections
While steroid injections can be effective for managing pain and inflammation in various musculoskeletal conditions, they are not always the first-line treatment. Several alternatives exist, each with its benefits and considerations:
Conservative Treatments
- Physical Therapy: A cornerstone of musculoskeletal treatment, physical therapy can help improve strength, flexibility, and function while reducing pain.
- Lifestyle and Activity Modifications: Adjusting daily activities, ergonomics, or exercise routines can often alleviate symptoms without medication.
- Oral Anti-inflammatory Medications: Non-steroidal anti-inflammatory drugs (NSAIDs) can provide systemic relief for inflammation and pain.
Alternative Therapies
- Shockwave Therapy: Particularly effective for tendon problems such as plantar fasciitis, tennis elbow, and Achilles tendinitis.
- Acupuncture: Some patients find relief through this traditional Chinese medicine technique.
- Massage Therapy: Can help reduce muscle tension and improve circulation in affected areas.
Alternative Injectable Treatments
- Hyaluronic Acid Injections: Often used for osteoarthritis, especially in the knee, to improve joint lubrication.
- Platelet-Rich Plasma (PRP): Utilizes the patient’s own blood components to promote healing and reduce inflammation.
- Arthrosamid: A new injectable treatment for osteoarthritis that forms a cushion-like gel within the joint.
- Prolotherapy: Involves injecting an irritant solution to stimulate the body’s healing response.
It’s important to note that these alternatives are often most effective when combined with other treatments. For example, steroid injections with physiotherapy can yield better results than either approach alone. What works best can vary from person to person, and it may take some trial and error to find the most effective approach for managing your condition.
Post-Injection Care and Recommendations
After receiving a steroid injection, it’s important to:
- Rest the injected area for 24-48 hours
- Avoid strenuous activities for a few days
- Monitor for any signs of infection or unusual reactions
- Avoid driving after a steroid injection.
Conclusion
Steroid soft tissue injections offer a valuable treatment option for many patients suffering from inflammatory conditions and chronic pain. They provide quick relief and can significantly improve quality of life.
However, like all medical treatments, they come with potential risks and limitations. It is important to have a discussion with your doctor about the benefits, risks, and alternatives before deciding on steroid injections. With proper use and management, these injections can be an effective tool in managing pain and improving function. While steroid injections can provide significant relief, they’re often part of a broader treatment plan that may include other therapies and lifestyle modifications. Always follow your healthcare provider’s recommendations for the best outcomes in managing your condition.
FAQ
Further reading:
https://www.nhs.uk/conditions/steroid-injections
https://www.nice.org.uk/guidance/ng226/chapter/Rationale-and-impact

Dr M Siebachmeyer
Musculoskeletal radiologist based at St Georges Hospital, London.
References
[1] A. Ocejo and R. Correa, “Methylprednisolone. [Updated 2024 Aug 11],” xPharm: The Comprehensive Pharmacology Reference, pp. 1–6, Aug. 2024, doi: 10.1016/B978-008055232-3.62167-1.
[2] J. L. del Cura and J. L. del Cura, “Editorial Comment: Corticosteroid Injections Are Safe, but They Have Side Effects That Must Be Known and Explained,” https://doi.org/10.2214/AJR.23.30780, vol. 222, no. 3, Jan. 2024, doi: 10.2214/AJR.23.30780.
[3] S. I. Kamel, H. G. Rosas, and T. Gorbachova, “Local and Systemic Side Effects of Corticosteroid Injections for Musculoskeletal Indications,” American Journal of Roentgenology, vol. 222, no. 3, Mar. 2024, doi: 10.2214/AJR.23.30458/ASSET/IMAGES/LARGE/23_30458_05D_CMYK.JPEG.
[4] T. E. McAlindon et al., “Effect of Intra-articular Triamcinolone vs Saline on Knee Cartilage Volume and Pain in Patients With Knee Osteoarthritis: A Randomized Clinical Trial,” JAMA, vol. 317, no. 19, pp. 1967–1975, May 2017, doi: 10.1001/JAMA.2017.5283.
[5] R. Kijowski, “Risks and Benefits of Intra-articular Corticosteroid Injection for Treatment of Osteoarthritis: What Radiologists and Patients Need to Know,” https://doi.org/10.1148/radiol.2019192034, vol. 293, no. 3, pp. 664–665, Oct. 2019, doi: 10.1148/RADIOL.2019192034.
[6] A. Guermazi, D. J. Hunter, and M. Kloppenburg, “Debate: Intra-articular steroid injections for osteoarthritis – harmful or helpful?,” Osteoarthritis Imaging, vol. 3, no. 3, p. 100163, Sep. 2023, doi: 10.1016/J.OSTIMA.2023.100163.
[7] J. Bucci et al., “Progression of Knee Osteoarthritis With Use of Intraarticular Glucocorticoids Versus Hyaluronic Acid,” Arthritis & Rheumatology, vol. 74, no. 2, pp. 223–226, Feb. 2022, doi: 10.1002/ART.42031.
[8] A. F. Buyuk, E. Kilinc, I. Y. Camurcu, S. Camur, H. Ucpunar, and A. Kara, “COMPARED EFFICACY OF INTRA-ARTICULAR INJECTION OF METHYLPREDNISOLONE AND TRIAMCINOLONE,” Acta Ortop Bras, vol. 25, no. 5, p. 206, 2017, doi: 10.1590/1413-785220172505172581.
[9] K. D. Garvey, M. J. Solberg, A. Cai, and E. G. Matzkin, “Efficacy of corticosteroid injection for subacromial impingement syndrome,” Ann Jt, vol. 3, no. 0, pp. 62–62, Jul. 2018, doi: 10.21037/AOJ.2018.07.01.